Did not match into residency? Find out what went wrong and how IMGs can rebuild a stronger application for the next match cycle.
Updated March 17, 2026
Table of Contents
The email arrives. You read it once, then again. The words don’t change. You did not match into residency as an IMG, and right now that’s the only fact your brain can hold.
Take a breath. You already know the path to US residency is steeper for an international medical graduate than for US-trained colleagues. You’ve cleared ECFMG certification, sat USMLE steps while navigating visa headaches, and put serious money and years into this. The disappointment is real.
But it’s not the end. For thousands of IMGs before you, this detour led somewhere, often to a career in American medicine that turned out better than the original plan. In this guide, we’ll work through exactly what to do when you don’t match into residency as an IMG; how to figure out what went wrong, and how to build a stronger application for the next cycle.
Understanding the IMG Match Reality
Start with the facts. The 2025 Main Residency Match results show continued strong IMG performance, with some important nuances.
2025 Match Data for IMGs:
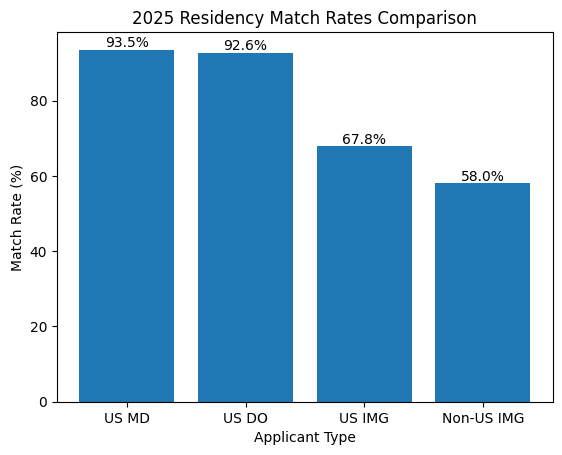
- Total IMGs matched: 9,761 secured first-year positions in accredited US GME programs
- Non-US citizen IMGs: 6,653 matched (58% match rate)
- US citizen IMGs: 3,108 matched (67.8% match rate)
- IMGs now make up more than a quarter of all matched applicants
Compare that to US MD seniors who matched at 93.5% and US DO seniors at 92.6%. The gap is real. As an IMG, you’re playing a harder game. But the NRMP data also shows this: nearly 10,000 IMGs matched in one cycle alone. Thousands do it every year. You can be one of them next cycle
Immediate Steps: The First 48 Hours After Not Matching
Allow Yourself to Grieve — Briefly
You’ve worked years or some of your for decades, toward this. You’ve sacrificed a lot: time away from family, real financial cost, navigating a foreign healthcare system, overcoming language and cultural barriers. The disappointment is valid.
Feel angry, frustrated, sad, embarrassed — whatever comes. Talk to people you trust, whether they’re in the US or back home.
Then set a deadline. Give yourself 48 hours maximum to process it. After that, shift into problem-solving mode. As an IMG, you don’t have the luxury of extended self-pity; the next cycle moves faster than you’d expect.
Connect with Your US Mentors and Network
If you rotated at US hospitals, built relationships through observerships, or connected with US physicians at any point, this is the moment to use those relationships. Send honest emails explaining your situation and asking for guidance. Most physicians who’ve been through training will help if they can.
Resist the Urge to Isolate
The instinct after a setback like this is to withdraw. You might feel ashamed to face classmates, embarrassed to tell your family back home, or uncomfortable about the investment your parents made. Fight this hard.
Isolation leads to rumination. Rumination leads to inaction. Stay connected in the US and at home. Let people show up for you. You’ll be surprised how many will.
Next Analyze why you did not match into residency
Once the shock wears off, sit down and figure out exactly what went wrong. Not a quick excuse, a real, honest look at why you didn’t match. This is the most important work you’ll do all year

Quantitative Metrics & Board Scores
This is the initial, objective filter residency programs use to manage application volume
| Potential Reason | Why It’s a Problem | How to Overcome It |
|---|---|---|
| Step 2 CK score below specialty average | Used as a primary filter; there is a significant score gap between matched and unmatched applicants | Compare your score with NRMP Charting Outcomes. Apply to specialties where your score is competitive |
| Failed attempt on Step 1 | Major red flag suggesting knowledge or test-taking issues | Professionally explain circumstances, show improvement, and perform strongly in clinical rotations |
| Failed attempt on Step 2 CK | More serious than Step 1 failure in the pass/fail era | Pass Step 3 and demonstrate strong clinical knowledge through USCE and research |
| Applying with scores in bottom 10% | Very low statistical chance of matching | Apply to less competitive specialties like Family Medicine, Psychiatry, Pediatrics |
| Failing Step 3 (graduates) | Raises concern about readiness for residency | Pass Step 3 on first attempt to strengthen your profile |
| Gap since graduation (>3–5 years) | Many programs filter out older graduates | Target IMG-friendly programs and show recent clinical activity |
| No Step 2 CK score at application | Programs rely heavily on Step 2 CK post Step 1 pass/fail | Delay application or apply strategically to programs that don’t require it |
Application & Profile Weaknesses That Hurt IMG Residency Chances
| Potential Reason | Why It’s a Problem | How to Overcome It |
|---|---|---|
| Generic or “template” Letters of Recommendation (LoRs) | Program directors easily identify generic letters; they suggest lack of meaningful connection | Request strong, personalized letters and provide your CV and interaction summary to writers |
| Letter writer not well-known or outside the specialty | Letters from recognized specialists carry more weight than unknown physicians | Build relationships with faculty in your target specialty, especially those with strong reputations |
| Inconsistent or contradictory letters | Mixed messaging creates a fragmented applicant profile | Ensure all letters align with your overall narrative and strengths |
| Unexplained gap in education or work history (>6 months) | Raises concerns about productivity and clinical skills decline | Clearly explain them in your application |
| Lack of research in research-heavy specialties | Fields like Orthopedics, Dermatology, Plastics value research heavily | Pursue research roles, publications, or a dedicated research year |
| Generic personal statement | Fails to show motivation or alignment with the specialty/program | Write a personalized story connecting your experiences to your chosen field |
| Personal statement errors (spelling/grammar) | Indicates lack of attention to detail | Get multiple reviews and proofread thoroughly |
| Superficial extracurricular activities | Shows lack of depth and commitment | Focus on meaningful experiences and reflect on what you learned |
| No letter from chosen specialty | Signals weak commitment to the field | Obtain at least one or two LoRs from your target specialty |
| Unprofessional social media presence | Programs may screen candidates online | Clean up or privatize social media accounts |
| Negative comments in MSPE (Dean’s Letter) | Professionalism issues are major red flags | Address concerns directly and demonstrate improvement through new experiences |
| Applying without ECFMG certification (IMGs) | Many programs require certification before considering applications | Complete certification before applying |
| Not explaining “why this region” | Programs prefer candidates likely to stay long-term | Highlight geographic ties or explain your interest in the region |
| Lack of volunteer or community service | Especially important for primary care specialties | Engage in meaningful service, particularly with underserved communities |
| Over-emphasis on prestige without substance | Can appear arrogant and unfocused | Emphasize fit, contribution, and learning goals instead of prestige |
Application Strategy Mistakes That Reduce Match Chances
| Potential Reason | Why It’s a Problem | How to Overcome It |
|---|---|---|
| Poor use of program signals | Wasting signals on reach programs reduces visibility at realistic target programs | Use signals strategically where you have geographic ties or competitive stats |
| Top-heavy rank order list (ROL) | Ranking mostly competitive programs increases risk of going unmatched | Create a balanced list with reach, target, and safety programs |
| Too narrow geographic preference | Limiting locations reduces interview opportunities in a national match | Stay geographically flexible to maximize chances |
| Insufficient number of applications | Fewer applications lead to fewer interviews and lower match probability | Apply broadly to a diverse mix of programs (80–150+ depending on specialty) |
| Applying to only one competitive specialty | Highly competitive specialties have low match rates for IMGs | Apply to a backup specialty where your profile is stronger |
| Not applying to enough safety programs | Lack of safer options increases risk of not matching | Include programs where your stats are above average |
| Applying late in the cycle | Late applications are disadvantaged in rolling review systems | Submit your application at least 2 days before programs start reviewing the applications |
| Ignoring new or less-known programs | These programs often have fewer applicants and higher acceptance chances | Target newly accredited or less popular programs |
| Not applying to preliminary or transitional years | Missing backup options can leave you unmatched entirely | Apply to both categorical and preliminary positions |
| Misunderstanding visa requirements (IMGs) | Applying to programs that don’t sponsor your visa wastes applications | Verify visa policies (J-1 vs H-1B) before applying |
Interview Mistakes That Cause IMGs to Go Unmatched
| Potential Reason | Why It’s a Problem | How to Overcome It |
|---|---|---|
| Poor interview performance (awkward, nervous, arrogant) | Programs prioritize interpersonal skills and teamwork | Practice with mock interviews, record yourself, and get structured feedback |
| Failing the “vibe check” or not appearing as a team player | Programs assess cultural fit and collegiality | Research program culture and demonstrate enthusiasm and teamwork |
| Unable to explain application weaknesses | Defensive or vague answers raise red flags | Prepare honest, structured responses showing growth and improvement |
| Not expressing genuine interest in the program | Programs rank candidates lower if interest seems weak | Send personalized thank-you notes and follow-up emails |
| Committing a Match violation | Dishonesty or pressure violates NRMP rules | Understand Match rules and communicate professionally without false promises |
| Asking poorly researched or inappropriate questions | Signals lack of preparation and interest | Prepare thoughtful, program-specific questions |
| Being late to an interview | Indicates poor professionalism and reliability | Plan ahead and join or arrive 10–15 minutes early |
| Poor body language (virtual or in-person) | Non-verbal cues can signal disinterest or lack of confidence | Practice posture, eye contact, and engagement through mock sessions |
| Speaking negatively about other specialties | Seen as unprofessional and narrow-minded | Stay positive and focus on your chosen specialty |
| Not sending a thank-you note | May signal lack of interest or professionalism | Send a concise, personalized thank-you email within 24 hours |
Reapplication Mistakes That Keep IMGs Unmatched
| Potential Reason | Why It’s a Problem | How to Overcome It |
|---|---|---|
| Inactive year off (no job, no research, no classes) | One of the biggest red flags; suggests lack of commitment and progression | Engage in clinical work (scribe, medical assistant), research, or meaningful volunteering |
| Lack of new, stronger LoRs for reapplication | Reusing old letters signals no improvement or growth | Secure new Letters of Recommendation from recent supervisors reflecting your progress |
| Isolating yourself and not seeking feedback | Lack of guidance leads to repeated mistakes | Stay connected with mentors, advisors, and medical school faculty for structured feedback |
| Ignoring NRMP data (Charting Outcomes) | Applying blindly reduces chances of matching | Use NRMP data to align your application with realistic specialty benchmarks |
| Failure to craft a new, positive narrative | Programs need to see growth after failure | Clearly demonstrate how you improved and why you are a stronger candidate now |
| Systemic barriers (socioeconomic or demographic factors) | Certain applicants face additional structural challenges | Seek mentorship programs and targeted resources to strengthen your application |
| Lack of US clinical experience | Programs prioritize candidates familiar with the US healthcare system | Gain USCE electives, externships, or research with US physicians |
Now you have your list. Here’s what to do with it

Go through each factor honestly. Then pick your top three to five that you feel was the reason why you did not match into residency. The areas where you fell furthest short. Not twenty things. Three to five.
Build your year around fixing those specifically. Every rotation, every research project, every volunteer hour should connect back to a real gap you identified.
Then bring your mentor into the conversation. Show them your assessment and your plan. They’ve seen this before and can tell you where your thinking is off.
This is a hard year. But it’s a navigable one. The doctors who made it through weren’t the ones who tried to fix everything at once — they were the ones who figured out exactly what went wrong and went after it.
Powerful Ways to Strengthen Your Application
Here are the areas that consistently separate matched IMGs from unmatched ones in the reapplication cycle.
1. Strategic Volunteering
Volunteering is one of the most underused tools available to unmatched IMGs. Done well, it serves several purposes at once: it builds connections, demonstrates commitment to service, develops clinical and interpersonal skills, and gives programs a reason to see you as someone who contributes rather than just competes.
Why Volunteering Matters for IMGs
There’s a useful shift in mindset here: instead of trying to out-compete other applicants, focus on what you can contribute. Programs can tell the difference. Volunteering demonstrates:
- Commitment to the community you want to serve
- Concerns beyond your own career advancement
- Developed empathy and interpersonal skills
- Initiative and leadership potential
The key take away: Choose something you actually care about. Programs can tell when an activity is genuine versus performed. Don’t pick a volunteering opportunity just because it looks good; pick one where you’ll actually show up and do real work.
2. Creating Measurable Societal Impact
Beyond volunteering, programs increasingly look for applicants who have created measurable impact, not just “I participated” but “I changed something.”
What Counts as Societal Impact
- Community health initiatives: Did you organize a health education campaign or start a screening program? How many people did you reach?
- Quality improvement projects: Did you identify a problem in a clinical setting and implement a fix? Quantify the improvement.
- Advocacy work: Did you push for health policy changes? Document your efforts and any outcomes.
- Public health research: Did your research affect practice or policy? Highlight the real-world implications.
- Health education: Did you create educational materials for patients? Track how far they reached.
Documenting Your Impact
When you write about creating community impact for medical residency applications, specifics are everything.
Weak: “Volunteered at a community clinic.”
Strong: “Organized a hypertension screening program at a community clinic serving 500+ uninsured patients, identifying 47 individuals with previously undiagnosed high blood pressure and connecting them to follow-up care.”
Numbers and specificity transform an activity from a line item into a story of real contribution.
3. Building a Professional Social Media Presence
Social media has become a legitimate tool for connecting with residency programs as an IMG — when used correctly. This is not about going viral. It’s about being a recognizable, professional presence before interview season starts.
Why Social Media Matters for Residency Applicants
A well-managed presence lets you get on a program’s radar before interview invitations go out, build familiarity with programs and their cultures, stay informed about virtual open houses and events, demonstrate professional engagement in your specialty, and network with current residents and faculty.
How to Connect Without Being Annoying
The approach is subtle and professional. Sending cold emails asking about interview spots before applications even open is a quick way to get blacklisted. Instead:
Finding programs: Follow residency programs on Twitter/X, Instagram, and LinkedIn. Follow program directors and faculty — but don’t over-engage. Follow professional organizations in your specialty.
Engaging appropriately: Like and comment thoughtfully on program posts. Share relevant content with your own professional commentary. Participate in Twitter chats in your field. Attend virtual open houses and engage with real questions. After events, follow up with genuine, specific comments.
What to Post
Your own presence should reflect professionalism and authentic interest in medicine: articles relevant to your specialty with your own take, updates on your volunteer work or research, thoughtful responses to content from other professionals, your perspective as an international medical graduate when appropriate, and nothing unprofessional, political, or potentially controversial.
Staying Organized
Track your social media engagement in a spreadsheet: programs you follow, events attended, connections made. This keeps you consistent and prevents things from falling through the cracks.
4. Increasing Research Publications
Research has always mattered, but in the post-Step 1 pass/fail world it’s become more important than ever, especially for IMGs. The importance of research publications for IMG match success isn’t debatable anymore.
The Data
Research on orthopaedic surgery matching reveals patterns that apply broadly: matched US citizen IMGs had at least three times more publications than matched US MD seniors, and matched non-US citizen IMGs had roughly five times more. IMGs who matched had significantly more publications than those who didn’t. IMGs are already publishing at higher rates to compensate for other application gaps. You need to do the same.
What This Means for You
- Quantity matters: the more publications, the better. IMGs typically need significantly more than US graduates.
- Quality matters: first-author publications carry more weight. Specialty-specific journals are particularly valuable.
- Consistency matters: steady output over time shows ongoing commitment.
- Presentations count: abstracts and conference presentations add value to your CV.

The Reapplication Blueprint: Your Year-Long IMG Strategy
Secure your position.
Whatever path you choose, research, clinical rotations, volunteering — lock it in now. Research positions fill early. Clinical rotations need lead time. Don’t wait.
Address your weaknesses directly.
If scores were the issue, consider whether a specialty pivot makes more sense than trying again in the same field. If research was thin, find a productive lab or project. If clinical experience was limited, prioritize patient contact hours.
Start volunteering.
Identify opportunities that fit your interests and schedule. Commit consistently rather than sporadically. Document your activities and track your impact.
Begin research.
Reach out to potential mentors. Start with accessible projects — case reports, systematic reviews. Set publication goals for the year.
Cultivate new US mentors.
Your gap year should yield new relationships. Find faculty who can become genuine advocates. Work hard, stay present, ask thoughtful questions. These people will write your new letters.
Build a living CV.
Create a document that captures everything as it happens. Every publication, every volunteer hour, every meaningful patient interaction. Don’t wait until application season to reconstruct it.
Months 4–6: Application Overhaul
Rewrite your personal statement.
Your previous statement didn’t work. Write a new one. Address your IMG journey honestly and positively:
” When I didn’t match in 2025, I secured a research position at [US institution], volunteered at a community health center serving 200+ patients, and published two papers. These experiences deepened my understanding of [specialty] and confirmed my commitment to practicing in the US.”
Answer the unspoken questions in your statement:
Why are you committed to US practice?
What makes you ready for US residency now?
How do you contribute to diversity in medicine?
Secure new US letters of recommendation.
Do not reuse old letters. Your new experiences — research, volunteering, clinical work — should produce new writers who can speak specifically to who you are now and how you’ve grown.
Revise every section of your ERAS application.
New experiences, new publications, new skills, new perspective. The application should tell the story of someone who grew from a difficult experience.
Build your social media presence.
Start following programs and engaging professionally. Attend virtual open houses. Build familiarity with your target programs before applications open.
Research programs strategically.
Build a detailed spreadsheet of target programs: IMG-friendly history, program type, location, average scores of matched IMGs. Know where you have a realistic shot.
Months 7–9: Strategic Application
Apply broadly — very broadly.
Submit early. IMGs should apply to significantly more programs than US graduates:
Internal Medicine: 150–250 programs
Family Medicine: 100–200 programs
Pediatrics: 100–200 programs
Psychiatry: 100–150 programs
Competitive specialties: every IMG-friendly program that exists
Don’t spend money on programs with no IMG history, but don’t apply conservatively either.
Use signals wisely.
Research which programs value signals and use yours on programs where you have a realistic chance. Geographic ties — family in a region, prior training there — are worth signaling.
Network actively.
Attend virtual conferences and introduce yourself
Engage on social media professionally and consistently
Reach out to residents at target programs
Show genuine interest without pressure
Start interview prep now.
Not when invitations arrive — now. Practice with mentors, US physicians, or paid services. Record yourself. Watch for communication patterns that don’t land well. Prepare for the questions you know are coming.
Months 10–12: Interview Season
Nail the IMG interview.
You’ve prepared for this. Speak clearly and at a measured pace. Don’t apologize for your accent — own it, but make sure you’re understood. Show that you understand US healthcare, not just its clinical side. Express genuine enthusiasm for the specific program. Highlight your volunteer work and community impact. Talk about your research with specifics. Mention your professional social media engagement when relevant. Ask questions that show you’ve done your homework.
Handle the “Why you did not match?” question directly.
You will be asked in interview. Have a clean, honest, forward-looking answer ready:
“After my first application, I realized I needed to strengthen my candidacy. I spent this year doing research at [US institution], where I published two papers. I also volunteered at a community clinic serving underserved populations and have been actively engaging with the professional community online. These experiences confirmed my commitment and made me a much stronger candidate.”
Practice this until it sounds like you’re saying it for the first time, not reciting it.
Build your rank order list strategically.
Balance reaches, targets, and realistic options. For IMGs, “safety” programs are ones with strong IMG histories where your scores exceed their typical averages. Be honest with yourself about where you fit.
Frequently Asked Questions
How do I balance research, volunteering, and clinical experience?
Focus on quality over quantity. Deep engagement in two or three areas is better than superficial involvement in five. Choose activities that genuinely interest you and that, together, tell a coherent story about who you are as a future physician
What’s the most important factor for IMG success?
There’s no single factor. IMGs who match typically have: strong Step scores, recent US clinical experience, US-based letters that speak specifically to their skills, meaningful research output, demonstrated community involvement, and applications targeted to IMG-friendly programs. The combination matters more than any one piece.

Your Story Isn’t Over
The physicians who end up being the most resilient residents — the ones with the most empathy, the ones who handle hard conversations without flinching, many of them have faced exactly this. They know what it means to fail at something they worked hard for and get back up anyway. That’s not a small thing.
Your path as an international medical graduate has already asked more of you than most US-trained physicians will ever be tested on. You left your country, your family, familiar systems, and a career you’d already built, to pursue something harder in a foreign place. That took courage, and it didn’t disappear when the match results came in.
This year will have hard days. Days when you question whether it’s worth continuing. But if you use the time well, volunteer in ways that matter, create real impact in communities, build a professional presence, and publish research; you’ll come out the other side a stronger candidate and a more prepared physician.
In 2025, nearly 10,000 IMGs walked this path successfully. They published more. They volunteered more. They connected more. They kept going when it would’ve been easier to stop. You can do the same.
Your IMG residency match story isn’t finished. Keep writing it.
Found this useful? Share it with other unmatched IMG applicants who need to know they’re not alone. Bookmark it for reference throughout your reapplication year.
Also feel free to check our USMLE Cost Calculator & YOG: Risk Calculator
Ready to Apply? Let Medvily Guide You!
Medvily offers a complete suite of services including:
- Tutoring / Mentoring
- Clinical Electives
- Observerships & Externships
- Clinical Research
- Residency Application Support
- Mock Interviews & IV Prep
- Medical Licensing Support
Disclaimer: All trademarks referenced herein are the property of their respective owners. Medvily disclaims any affiliation, sponsorship, or endorsement by such trademark owners or their affiliated companies. The information provided is for general informational purposes only.



